Cognitive Behavioral Therapy for Insomnia
- by Rose MacDowell
- Updated: April 6, 2023
Table of Contents
Insomnia is the world’s most common sleep disorder, and affects up to half the human population. The disorder is characterized by the inability to sleep, even when given the opportunity to do so. Symptoms of insomnia — difficulty falling asleep, staying asleep, and/or falling back to sleep — may persist for months or years.
One of the most effective treatments for chronic insomnia is a protocol intended to modify actions, thoughts, and sleep patterns that contribute to the inability to sleep. The protocol is known as Cognitive Behavioral Therapy for Insomnia, and studies show it may improve sleep in 80% or more of patients who complete treatment.
Cognitive
Conscious intellectual activity such as thinking, reasoning, or remembering.
Note: The content on Sleepopolis is meant to be informative in nature, but it shouldn’t take the place of medical advice and supervision from a trained professional. If you feel you may be suffering from any sleep disorder or medical condition, please see your healthcare provider immediately.
Cognitive Behavioral Therapy for Insomnia (CBT-I)
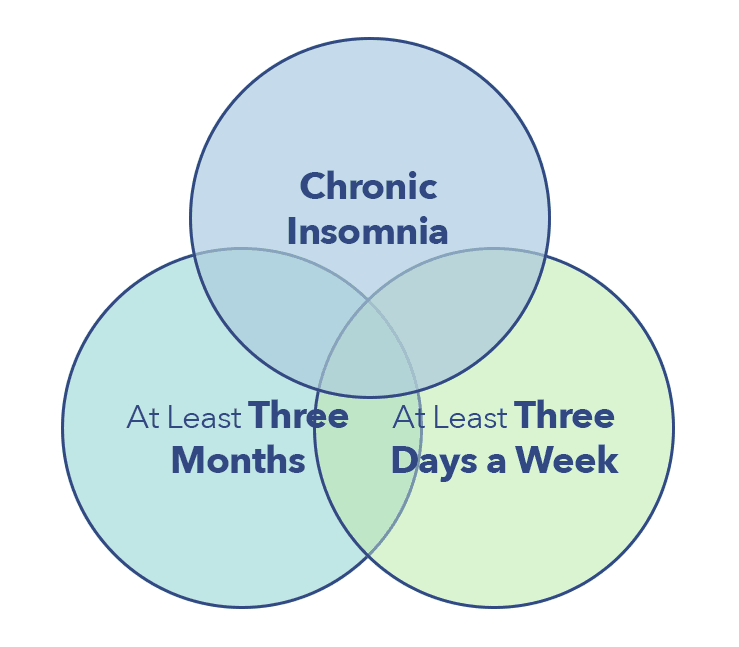
One in four Americans experiences insomnia each year, while 10% suffer from the disorder chronically. Most people with insomnia suffer from short-term insomnia symptoms that resolve on their own within days or weeks. To be considered chronic, symptoms must continue for at least three consecutive months, and occur at least nights each week. (1)
 Insomnia is more than just an inconvenience. When chronic, the disorder can have a significant impact on physical and emotional health. Recent research shows that insomnia may be linked to depression, anxiety, and other mood disorders. (2) Insomnia can also cause serious medical issues, from metabolic dysfunction to increased risk of stroke. Early and effective treatment of the disorder is essential for optimal psychological and physical well-being.
Insomnia is more than just an inconvenience. When chronic, the disorder can have a significant impact on physical and emotional health. Recent research shows that insomnia may be linked to depression, anxiety, and other mood disorders. (2) Insomnia can also cause serious medical issues, from metabolic dysfunction to increased risk of stroke. Early and effective treatment of the disorder is essential for optimal psychological and physical well-being.
While short-term insomnia symptoms — also known as acute insomnia — are typically related to a stressor or other temporary circumstance, chronic insomnia is nearly always a result of negative psychological associations with sleep and the sleeping environment.
Typical treatments for insomnia disorder include:

- Medications (3)
- Supplements of the sleep-promoting hormone melatonin
- Antihistamines and other over-the-counter sleep aids
- Behaviors intended to increase the relaxation response, such as yoga, deep breathing, and meditation
- Bright light therapy
- Lying passively in bed without trying to sleep
- Improved sleep hygiene
- Therapy for stress reduction
While such treatments have a place in the treatment of insomnia, none has been proven as effective as CBT-I. Cognitive behavioral therapy for insomnia is now the first-line treatment for chronic insomnia. It appears to be effective for all types of insomnia, regardless of severity, and including those associated with mood disorders.
Cognitive behavioral therapy is quite different from cognitive behavioral therapy not associated with a sleep disorder. The protocol involves several complementary components, and typically requires between three and eight sessions.
FAQ
Q: How does bright light therapy for insomnia work? A: Bright light helps to reset the circadian rhythm by sending powerful wakefulness cues through the retina to the brain.Initial Evaluation
To determine if cognitive behavioral therapy is the appropriate treatment for a case of insomnia, a doctor will usually conduct an evaluation. Most evaluations involve a detailed sleep and medication history, as well as an assessment of physical and psychiatric health. (4)
One of the goals of a sleep evaluation is to detect any medical or mood disorders that may be contributing to the inability to sleep. These might include:
- Depression
- Anxiety
- A circadian rhythm disorder
- Another sleep disorder such as sleep apnea or restless legs syndrome
- A medical condition such as hyperthyroidism, asthma, or Parkinson’s Disease
- Use of certain medications or other drugs
A full evaluation may also require keeping a sleep diary and filling out the Epworth Sleep Questionnaire. The Epworth Sleep Questionnaire asks patients to rate their likelihood of falling asleep during a number of activities, including driving, resting after lunch, and carrying on a conversation.

A doctor may also ask for the patient’’s assessment of their own sleep quality, ability to function during the day, quality of life, and beliefs and attitudes about sleep. Sleep studies are often conducted when evaluating other sleep disorders, but are generally not needed to diagnose chronic insomnia.
Once a diagnosis of chronic insomnia is made, CBT-I is typically suggested as the preferred treatment. Cognitive behavioral therapy for insomnia is quite different from therapy not associated with a sleep disorder. The protocol involves several complementary components, and usually requires between three and eight sessions.
Circadian rhythm disorders
Circadian rhythm disorders are sleep disorders that occur when the circadian rhythm -- or body's internal clock -- becomes desynchronized, causing irregular sleep patterns.
Stimulus Control Therapy (SCT)
One of the essential elements of CBT-I is stimulus control therapy, or SCT. This part of the protocol is designed to reduce negative associations regarding sleep and the sleep routine. “Stimulus” refers to anything that can cause a physical or emotional response. In the case of chronic insomnia, the stimulus is typically behaviors or thoughts that can activate the nervous system, cause anxiety, or serve as a cue for wakefulness.
For many people with chronic insomnia, the bed has become a place for activities such as reading or television-watching, as well as planning or worrying about upcoming events. Bed and the bedtime routine may also have become psychologically linked with the inability to sleep. Stimulus control therapy is designed to strengthen associations with the bed as a place to sleep. (5)

The SCT protocol can help alleviate negative conditioning through the following behaviors:
- Go to bed only when sleepy
- Go to sleep and wake up at the same time every day, even on weekends
- If unable to sleep after approximately ten minutes (don’t clock watch! Just guesstimate), get up and wait to feel sleepy in another room
- Use the bed for sleep and sex only
- Once in bed, don’t look at the clock
Stimulus control therapy also requires the avoidance of naps, which can reduce the drive to sleep and make falling asleep at a consistent time more difficult.
FAQ
Q: What is the sleep drive? A: An internally regulated system that increases over the course of a day and with the passage of time. The sleep drive diminishes with sleep and exposure to light.Sleep Restriction Therapy
People with chronic insomnia typically spend a significant amount of time attempting to sleep. Sleep restriction therapy limits time in bed to the average number of hours spent sleeping. This part of the protocol helps to increase the efficiency of sleep and reduce time spent lying awake. (6)
Basics of sleep restriction include:
- Restricting time in bed to the average total sleep time. For example, if the average amount of time spent sleeping is 5 1/2 hours, bedtime would begin at 12:30 am and end at 6 am. Sleep restriction therapists typically recommend going to bed later and waking at a normal time rather than going to bed earlier and waking earlier.
- It’s important to note that sleep restriction therapists will not limit you to less than 5 hours in bed even if you’re sleeping less than that each night.
- Increasing or decreasing time in bed by 15 minutes each week.
- Increasing time in bed only when sleep efficiency increases and benefits of therapy become apparent.
- Decreasing time in bed if still lying awake.
The sleep restriction protocol helps to weaken the mental association between the bed and the inability to sleep. Though restricting the amount of time available to sleep may initially seem counter-productive, sleep restriction can be remarkably effective at restoring the natural drive to sleep. This in turn reinforces the psychological connection between the bed and healthy sleep patterns.
The sleep restriction protocol helps to weaken the mental association between the bed and the inability to sleep. Though restricting the amount of time available to sleep may initially seem counter-productive, sleep restriction can be remarkably effective at restoring the natural drive to sleep. This in turn reinforces the psychological connection between the bed and healthy sleep patterns.
Relaxation training
The goal of the relaxation training part of the protocol is to help insomnia sufferers reduce anxiety and physical tension. The training is designed to reduce activation of the nervous system and promote sleep. Inappropriate arousal of the nervous system can cause the release of stress hormones such as cortisol and adrenaline, and cause or worsen insomnia.

Relaxation techniques typically involve breathing, guided imagery, meditation, and progressive relaxation of the muscles. (7) Hypnosis or biofeedback may also be included as part of the training protocol. Using data about such vital signs as heart rate, blood pressure, and body temperature, biofeedback can help insomnia sufferers recognize and reduce symptoms of physical tension throughout the day and at bedtime.
Cognitive behavioral therapy
The therapy piece of the CBT-I protocol focuses on changing dysfunctional beliefs and attitudes about sleep. (8) A cognitive behavioral therapist can help a patient identify thought patterns that contribute to insomnia. These might include thoughts of being unable to work without sufficient sleep, or fears of becoming sick after a sleepless night. The therapist may challenge these beliefs by pointing out the many times the insomnia sufferer performed well at work or remained healthy after lying awake the night before.
Specialists in CBT-I also focus on treating the anxiety that underlies many cases of chronic insomnia. Keeping a written record of sleep-related thoughts and feelings may help reveal dysfunctional thought patterns so they can be replaced with ways of thinking that promote healthy sleep.
Sleep hygiene
“Sleep hygiene” is the term for a set of actions and lifestyle changes intended to promote healthy sleep. Good sleep hygiene can help correct habits that contribute to delayed or fragmented sleep. The recommendations vary, but typically consist of suggestions designed to eliminate causes of poor sleep.
Though sleep hygiene by itself is generally not an effective treatment for chronic insomnia, insomnia sufferers may benefit from improving the sleep environment and simple sleep-related behaviors. Sleep hygiene basics include:
- Abstaining from alcohol and caffeine in the hours before bed
- Creating a dark, quiet, and cool sleeping environment
- Avoiding evening use of electronics that emit blue light, including smartphones, tablets, and computers
- Exercising regularly in the morning or afternoon
- Avoiding heavy meals before bed
In combination with the CBT-I protocol, practicing good sleep hygiene may help eliminate habits that exacerbate insomnia and disrupt sleep patterns.
Last Word from Sleepopolis
To those who suffer from it chronically, insomnia may seem like an intractable problem. Anxiety associated with the inability to sleep often compounds the problem, making healthy rest even more difficult to attain. Fortunately, treatments exist for those who suffer from this frustrating disorder. Cognitive behavioral therapy for insomnia may be effective even for cases that have persisted for months or years.
The protocol is now widely accepted as the first-line treatment for chronic insomnia, and practitioners are becoming more numerous. Though it may take time and discipline, the success rate for cognitive behavioral therapy for insomnia may exceed that of medications, and endure far longer after treatment is completed.
References
- Michael H Bonnet, PhD., Evaluation and diagnosis of insomnia in adults, UptoDate, Aug.15, 2018
- Baglioni C, Battagliese G, Feige B, Spiegelhalder K, Nissen C, Voderholzer U, Lombardo C, Riemann D., Insomnia as a predictor of depression: a meta-analytic evaluation of longitudinal epidemiological studies, Journal of Affective Disorders, Dec. 2011
- Lie JD, Tu KN, Shen DD, Wong BM., Pharmacological Treatment of Insomnia, Pharmacy & Therapeutics, Nov. 2015
- Schutte-Rodin S, Broch L, Buysse D, Dorsey C, Sateia M., Clinical Guideline for the Evaluation and Management of Chronic Insomnia in Adults, Journal of Clinical Sleep Medicine, Oct. 15, 2008
- Richard R. Bootzin, Dana Epstein, James M. Wood, Stimulus Control Instructions, Case Studies in Insomnia, 1991
- Miller CB, Espie CA, Epstein DR, Friedman L, Morin CM, Pigeon WR, Spielman AJ, Kyle SD., The evidence base of sleep restriction therapy for treating insomnia disorder, Sleep Medicine Reviews, Oct. 2014
- Edinger JD, Wohlgemuth WK, Radtke RA, Marsh GR, Quillian RE., Cognitive behavioral therapy for treatment of chronic primary insomnia: a randomized controlled trial, JAMA, Apr.11, 2001
- Morin, CM, Cognitive-Behavior Therapy, Singly and Combined with Medication, for Persistent Insomnia: Acute and Maintenance Therapeutic Effects, JAMA, Mar.8, 2011
Subscribe Today!
Get the latest deals, discounts, reviews, and giveaways!
