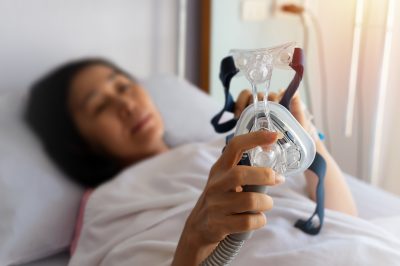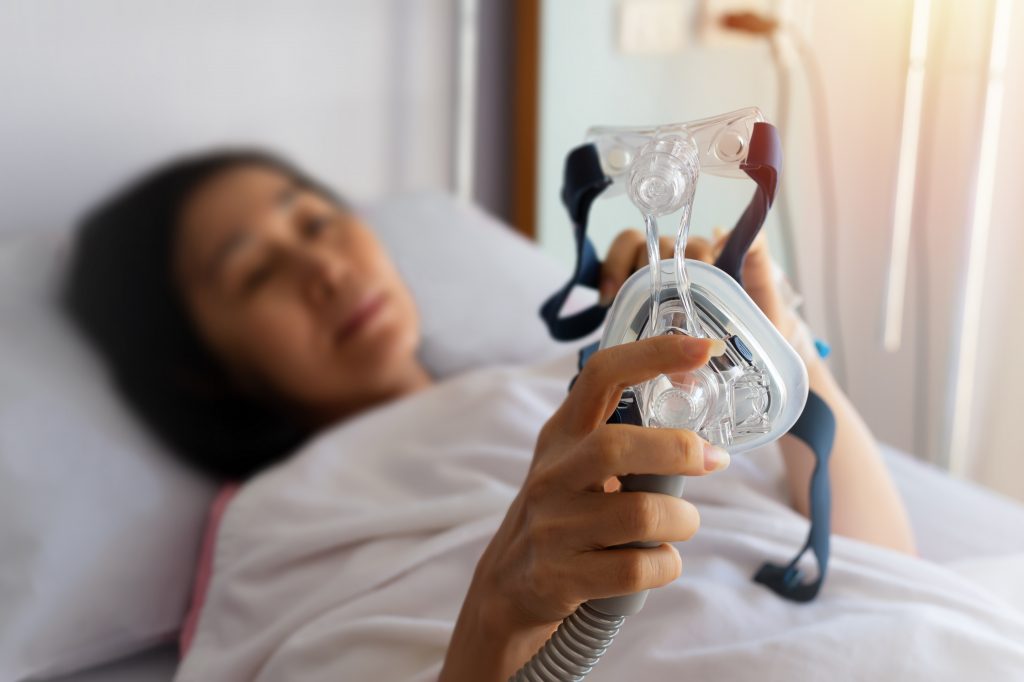
After a major, disruptive voluntary recall of sleep aid machines from Philips limited access to many of the devices for millions, users are on the hunt for alternatives to the machines.
For some, simply putting a large mask over your face, attached to various cords and tubes, and then trying to sleep is nearly impossible — especially for those who are claustrophobic. But for those suffering from snoring, sleep apnea, and related conditions finding a safe, reliable device is mandatory.
Challenges with CPAP machines
For some, a CPAP machine is essential and the most effective treatment for diagnosed sleep apnea, according to family physician Dr. Mike Sevilla at Family Practice Center of Salem in Ohio. Nobody with sleep apnea should suddenly stop using their CPAP machine without discussing alternatives with their doctor, for their own safety.
“CPAP masks can be bulky and uncomfortable to use. Many people also can’t tolerate the noise these machines make. Some find it hard to breathe with the air pressure the machine provides,” says Dr. Po-Chang Hsu, Medical Content Expert at Sleeping Ocean, says. “Additionally, CPAP devices aren’t ideal for people who travel a lot and are usually heavy, bulky, and challenging to transport. It’s also worth mentioning that CPAP machines don’t always work, especially when dealing with central sleep apnea.”
It’s also key to consider how quickly you need change (if someone can’t sleep overnight without serious breathing issues, this is much more severe than a little snoring), and to align treatments with those concerns with your doctor’s help. And for the many now scrambling to find safer devices because of the Philips recall, there are some options.
Alternatives to CPAPs
From jaw-angling devices to lifestyle changes, there are alternatives to CPAP machines that might help for some conditions. Here are some recommendations from the experts.
Mandibular Advancement Devices
While retainers and mouthguards may seem like a thing of your past, taking you back to teen years or sports games, they also play a role in snoring and relating issues. Mandibular Advancement Devices splint or stabilize the throat and airway, reducing their ability to collapse which is associated with Sleep Apnea, according to Dr. Mitchell Levine, diplomat of the American Board of Orthodontics and the American Board of Dental Sleep Medicine. They do this by pushing the jaw into a more “forward” position, which he compares to taking a pipe and reinforcing the airway by making it stronger, and less likely to fall back on itself.
Levine says this option is best for those with mild or moderate, not severe, sleep apnea. He’s seen a rise in requests for these devices from patients, especially as their CPAP machine providers struggle with the recall but also with supply chain issues. He emphasizes that patients have a higher chance of keeping mandibular devices in their mouths all night, versus taking off a CPAP machine halfway through the night due to discomfort, making it an important option to consider.
Changing position
You might be a dedicated back, side, or belly sleeper, but your position might also impact your overnight health and breathing quality. Hsu says, “Sleeping styles have a lot to do with breathing and snoring. Each position results in different airway pressure levels that may aggravate or alleviate snoring.” He adds that back sleeping especially makes the tongue and the soft palate fall back, potentially obstructing airways and adding to snoring. “Back sleeping may also put more pressure on the throat muscles. This can also lead to breathing difficulties and snoring.”
Orofacial therapy
Orofacial therapy is basically like physical therapy for your mouth, throat, facial muscles, and surrounding structures. Recent studies have shown this type of therapy to improve oxygen saturations, reducing snoring and sleep apnea effects, including daytime sleepiness. This therapy can be extremely effective, with some research indicating adults decreased their sleep apnea index (called apnea-hypopnea index) by 50% and children by 62%. It can also be used alongside other treatments, such as the CPAP or position changes.
Lifestyle changes
Improving diet, nutrition, and therefore seeing potential weight loss can quickly improve sleep apnea and snoring, according to Hsu. “Such lifestyle changes as exercise, weight loss, and a proper diet can be an effective treatment if one’s sleep apnea isn’t severe,” he says. “It shouldn’t take too long in this scenario to start noticing improvements. In other cases, these adjustments must be combined with other treatments (a CPAP machine, medications, or any other solution one’s doctor might recommend).”
Surgery, in severe cases
For some, snoring is just an annoyance to their partners and can disturb their sleep. For others, breathing concerns during sleep indicate more serious health problems that can sometimes be solved through surgical procedures. “They include nasal, palate, tongue, and jaw surgeries; tonsil or adenoid removal; skeletal surgery; palate implants; nerve stimulation, etc. One of the most common treatments for sleep apnea is UPPP – Uvulopalatopharyngoplasty,” Hsu says. “During the procedure, the doctor removes a part of one’s palate, tonsils, and often uvula. This can help free up the airways to maintain steady, snore-free breathing during sleep.” Doctors will likely turn to other options before suggesting surgery. “Patients might also consider getting surgery when sleep apnea seriously interferes with their daily lives. For instance, it may cause chronic sleep deprivation, affecting their health, mood, and productivity.”
All of our experts emphasize discussing options with your doctor before making any changes.